Dissolving the Problem: How Biodegradable Stents Are Transforming Cardiovascular Care
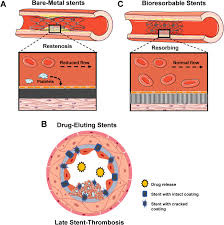
Coronary artery disease (CAD) remains the leading cause of death worldwide, responsible for over 9 million deaths annually according to the World Health Organization. Traditionally, one of the most effective treatments has been the use of metal stents—small mesh tubes inserted into arteries to restore blood flow. However, despite their life-saving utility, permanent metallic stents come with long-term complications, including chronic inflammation, restenosis (re-narrowing of the artery), and the need for extended anti-clotting therapy.
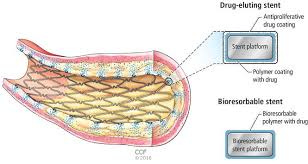
In response to these limitations, a new generation of medical devices has emerged: biodegradable stents, also known as bioresorbable vascular scaffolds (BVS). These stents are designed to provide temporary support to blood vessels and then harmlessly dissolve within the body over time. The concept offers an elegant solution—support when it’s needed, and disappearance when it’s not.
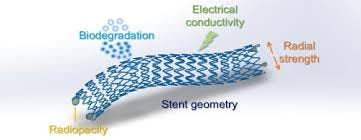
The principle is simple. Once a biodegradable stent is implanted, it works like a traditional stent, propping open the artery to maintain blood flow. But over a period of 12 to 36 months, it gradually degrades into carbon dioxide and water or other naturally occurring substances, depending on the material used. Most are made from polylactic acid (PLA), a material commonly used in absorbable sutures, though magnesium-based alloys have also gained attention for their faster dissolution and stronger mechanical support.
Clinical data on biodegradable stents has been mixed but is improving with second-generation technologies. The first major bioresorbable stent to receive CE mark approval in Europe and FDA approval in the U.S. was Abbott’s Absorb BVS in 2016. Early enthusiasm was dampened by studies like ABSORB III, which showed higher rates of thrombosis and adverse cardiac events when compared to traditional drug-eluting stents (DES). However, the issues were largely attributed to thicker struts, improper deployment, and poor patient selection.
Since then, manufacturers have refined stent design, reduced scaffold thickness, and introduced advanced imaging tools like optical coherence tomography (OCT) to improve placement accuracy. A 2023 meta-analysis published in Circulation found that next-generation bioresorbable stents, such as the Magmaris (Biotronik) and Firesorb (MicroPort), demonstrated comparable safety and efficacy to standard DES when used in properly selected low-risk patients.
The advantages of bioresorbable stents extend beyond mechanical support. Because they leave no permanent implant, they allow the vessel to heal more naturally and may reduce the long-term need for dual antiplatelet therapy. In younger patients, this could mean avoiding complications associated with lifelong metal implants. There’s also growing interest in their use for peripheral artery disease (PAD) and even pediatric cardiology, where growing bodies would otherwise outgrow fixed devices.
Economically, biodegradable stents remain more expensive than their metal counterparts, typically ranging from $2,000 to $3,500 per unit compared to $1,000 to $1,500 for a standard DES. However, proponents argue that reduced long-term complications and fewer follow-up interventions could lead to lower lifetime treatment costs. Ongoing cost-effectiveness trials in Europe and Japan are expected to provide further clarity over the next few years.
Despite their promise, biodegradable stents are not a one-size-fits-all solution. Their use currently makes the most sense in specific populations—particularly younger, low-risk patients with straightforward coronary lesions. In more complex cases, the robust radial strength of metal stents still offers a clinical edge. Moreover, long-term follow-up beyond five years is still sparse, leaving open questions about late-stage vascular remodeling and very late thrombosis.
That said, the potential of bioresorbable technology continues to inspire innovation. Research teams are developing smart stents that not only dissolve but also deliver localized drugs or monitor hemodynamics in real time. Some prototypes even integrate bioelectronic sensors powered by energy harvested from arterial motion.
In a medical field where permanence often comes with hidden costs, the ability to implant a device that does its job and then quietly disappears could be revolutionary. As technology matures, biodegradable stents may well shift from niche applications to standard practice, especially as the focus of cardiovascular care moves toward minimizing intervention while maximizing recovery.


Thoughts?
Really interesting read. Are there any updates on how these stents are performing in real-world settings beyond clinical trials?